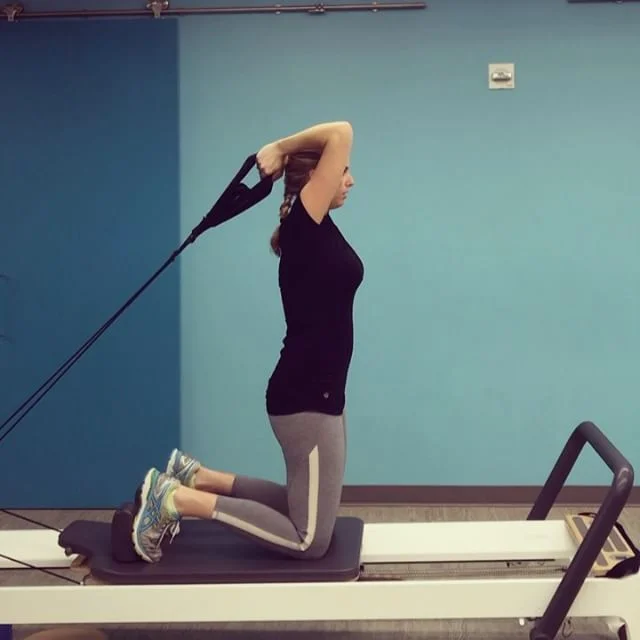Neck and low back pain.
Rehabilitation of sporting injuries.
Recovery post surgery.
Pre-natal & post-natal pilates.
Physiotherapy / Physical Therapy
Sian Smale is an Australian-trained Musculoskeletal Physiotherapist and Clinical Pilates Instructor. As a Physiotherapist, Sian has a keen interest in helping people with neck and back pain, headaches and sporting injuries. Growing up, Sian enjoyed many sports including swimming, volleyball, field hockey and tennis. More recently yoga, cycling, and snowboarding/skiing have captivated her time.
Sian lives in Melbourne and works at Physica Spinal and Physiotherapy Clinic. Sian uniquely blends Australian and American best practices together due to her experience working in San Francisco as a licensed Physical Therapist for many years before returning to Melbourne with her family. In 2009, Sian was awarded a Bachelor of Physiotherapy from La Trobe University and 2013 awarded a Masters Degree in Musculoskeletal Physiotherapy from Melbourne University. Combining her love of sport, passion for manual therapy and training in Pilates, Sian is able to design individualized treatment programs and Pilates programs that truly focus on your goals and problems.
Clinical Pilates
In Clinical Pilates sessions, Sian focuses on individual, one-on-one sessions tailored to each client's goals and needs. These programs can involve a wide range of equipment from pilates reformers, Redcord, fitness balls, free weights and mat work. Sian completed her clinical pilates training through DMA (Dance Medicine Australia), and is a certified Functional Movement System instructor (FMS).
Physiotherapy Blog
Sian spent many years blogging on the Physiotherapy blog Rayner & Smale. Sian continues to enjoy reading peer-reviewed journal articles and formulating evidence-based approaches to assessment, yet family has been her priority recently over blogging.
Qualifications
Licensed Physiotherapist and APA-titled Musculoskeletal Physiotherapist in Australia 2009-current time
Licensed Physical Therapist in California 2017-2021
Clinical Pilates Instructor
Dry Needling Certification (Australia only) & Myofascial Decompression certification
CPR certified




.jpeg)